
Tongue function and its role in dental health is a hot topic at the moment.
Infant tongue-tie and its impact on dental, breathing, and sleep health have seen a recent spike in attention. The symptoms of an undiagnosed tongue tie can link to mouth breathing, poor sleep, sleep apnea, neck pain, digestive issues, and anxiety.
Many parents are seeking tongue-tie releases for their newborns to help a child to breastfeed. But what about those of us who didn’t get released earlier in life? Adult tongue-ties are a much less talked about procedure. There is now a growing group of health practitioners performing this procedure.
Adult tongue-tie release can be undertaken by dentists, oral surgeons, and ENTs.
Research in this field is limited due to it being a relatively new area of clinical focus. There is a need for clinical trials to measure outcomes vs risk of procedures. However, knowledge and experience of the potential health benefits of tongue-tie release is growing and far outweighs risks when carried out by an experienced practitioner. Many people are seeking adult tongue-tie release and seeing benefits.
I’ve written this blog to give you an overview of your options for oral restriction release.
I recently came across a case study on adult tongue-tie release. It’s useful because it describes the set of symptoms I often see in adults with tongue-tie. The patient is a Certified Practicing Speech Pathologist trained in orofacial myofunctional therapy.
Michelle’s story is one that many people may relate to and she has kindly shared her before and after tongue-tie experiences.
Tongue tie problems in adults
For one reason or another, tongue-ties became a lost part of the pediatric dentistry assessment. Midwives were known to clip a newborn’s tongue-tie at birth if spotted with a sharp fingernail. Retired pediatricians have reported a ‘thrive or die’ approach early in their careers. If newborns were found to have feeding or other issues they were routinely checked for tongue tie.
The second half of the 20th century saw a movement away from the practice of breastfeeding. It may have been caused by the rise of formula and bottle feeding, which together, made diagnosing a tongue tie as a long-lost art.
That means there are two to three generations that grew up with tongue-ties. It’s a large group of adults and could mean that you unknowingly have a tongue-tie.
Your tongue is such a crucial part of your body. The neuromuscular system is intertwined with the brain, digestive system, neck, spine, and teeth. To get an understanding, I recommend reading this blog on its role in breastfeeding and preventing braces.
Symptoms of tongue tie before surgery
Tongue tie symptoms in adults may be similar to those found in kids. But in adults, a tongue-tie may be underlying a broader set of conditions and diseases.
Let’s look at the tongue tie symptoms Michelle experienced.
Michelle had suffered symptoms all her life that may have been due to her life-long tongue-tie.
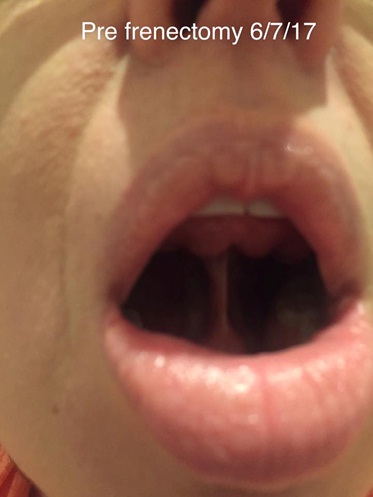
“I had a debilitating lack of energy. It was difficult to get through the work week. It would mean afternoon naps, and craving sugar to give her energy.
I was always a bad sleeper. This culminated in a diagnosis of snoring and obstructive sleep apnea. The sleep study showed an AHI (apnea-hypopnea index of 30).
I began CPAP treatment three years ago, of which brought my AHI down to 1-2. But it still didn’t make me feel rested.
CPAP helped a little bit, but I was still so tired that I could not entertain the idea of socializing through the week out of fear of losing sleep.
For most of my life, I had chronic neck and back pain. It would focus at a point on the right scapula and spread through the shoulder and thoracic area.
The pain also included my jaw joint. I had TMD which meant my jaw would open to the left and would click on the right 3 times and left 2. I’d wake in the morning with a sore jaw joint and I had chronic migraines.
The morning jaw pain was probably due to my teeth grinding at night. The daily mouth breathing seemed to give me sensitive teeth. I would often have a rush of tooth pain when I would drink cold water. I would go through a stick of lip chap in two weeks, on bad weeks it would be one because my lips were so dry during the day to which I now realize was due to mouth breathing.
In general, my sleep was light. I would wake with acid reflux and the feeling of ‘pressure.’ It would always be a struggle to get back to sleep, and this made a horrible cycle of being scared about being tired, and unable to sleep.
I was seeing a psychologist for anxiety.”
Michelle’s story is powerful because the symptoms are so common.
Here’s a summary of her symptoms before tongue-tie release:
- Brain fog, tiredness, lack of energy
- Frequent dry lips on a daily basis even though she used lip balm
- Waking up tired
- Afternoon naps
- Grumpiness and irritable
- Snoring
- Lisp as child
- Sleep apnea
- Chronic neck pain, back, and shoulder pain
- Jaw pain and audible jaw click and pain on opening
- TMD on her right-hand side – she would wake up with sore jaw joints
- Migraines
- Childhood lisp
- Diet food craving sugar
- Sugar cravings for energy
- Tooth sensitivity – rush of pain with water consumption
- Mouth breathing (air coming in on teeth)
- Teeth grinding
- Anxiety and depression
- Digestive issues and diseases
Am I Tongue Tied? How to identify oral restrictions
Does any of the above sound familiar? If you suffer any of these conditions, let’s go on to see a simple test that may reveal a tongue tie.
- Do a finger swipe under your tongue, is there a catch? It should be a smooth transition.
- Is there a visible flap of skin under the tongue? There should be no flap.
- Do you experience a strong gag reflex?
- Stick your tongue out, straight, now can you lift the tip without moving the rest of the tongue? You should be able to move the tip independently of the rest of the tongue.
- Open your mouth, as wide as it goes. Without moving or closing the jaw, can you reach the tip of your tongue to spot behind your upper front teeth? Your tongue should reach the spot behind your front teeth at FULL jaw opening.
- Can your tongue comfortably wipe across the outer sides of your upper and lower back teeth and reach where the gums connect with the cheeks?
- Can you move your lips side to side (lips closed) without moving the entire jaw? The lips should be able to move independently to the jaw. This may indicate a lip tie, which is a slap of skin between the lip and the gums inside the mouth. It’s similar to a tongue tie in that it can restrict full lip movement.
*There are other signs on the face and body that a well trained professional can assess as well as several related issues that stem from tongue restriction. These include airway, posture, and sleep and a practitioner can assess you beyond just appearance of the tongue.
Adult Tongue Tie Surgery Before and After
Before Tongue Tie Surgery
As a trained Orofacial Myofunctional Therapist, Michelle completed her own 8-week myofunctional therapy program surrounding her laser release. She worked under the guidance of Sandra Coulson from the Coulson Institute who she trained under. She then connected to the great team at Enhance Dentistry in Brisbane. The plan was that she would complete a further 2-week myofunctional therapy program before the release.
The general goals of myofunctional therapy are:
- Develop a nasal breathing pattern
- Correct rest posture of the tongue
- Guide closed lips resting position
The therapy includes using a sticky spot to help train the tongue to sit at the top of the mouth.
She reported the following benefits before tongue-tie surgery at week 4 of myofunctional therapy.
“I still found it uncomfortable to hold correct tongue posture. I was wearing four spots (spot, central upper, lateral) to encourage tongue posture on the roof of mouth but it was far too tight at the base of tongue and floor of the mouth.”
- Within 48 hours, she could perform nasal breathing comfortably while keeping the tongue to the spot
- Sleeping better, alert and better rested.
- Using less lip chap during the day as a result of using the spots indicating she breathing through her nose
- She had gained jaw stability and lip posture to keep the mouth together
- She reported waking up with tongue up with mouth open. Her lips and jaw didn’t have the strength to maintain a closed position, but she felt nasal breathing was occurring with the tongue up.
- She reported a soreness down the neck at the base of the skull. She attributes this to the tongue muscles straining to push the tongue up while her mouth posture was open.
- The rough rugae at the top of the mouth appear to have expanded. The skin appeared new due to tongue contact.
After tongue tie surgery
Michelle opted to have her oral restrictions released by laser.
“I had three releases (tongue, upper and lower lip ties) under the care of the amazing Dr. Marjan Jones (Dentist and director and The Tongue Tie Institute Australia) and her team. My 4 ties were submucosal tongue tie, clean-up of previously busted upper lip tie, lower lip tie and laser behind bottom front teeth. I chose to have a local anesthetic [as some patients choose topical anesthetic only]. I have since been under the Myofunctional guidance of the amazing Sarah Beach.
Of most interest to me was during the procedure, I could feel what I can only describe as ‘pings’ of muscle release as my TMJ tension, right middle scapula knife like pain, right side neck and middle of neck and shoulder right side pain all disappeared. Also noted immediately post release, TMJ has one small dull click, and my usual left deviation on opening was gone. My lateral neck twists extension could go past my shoulder (previously slightly in front of the shoulder.)”
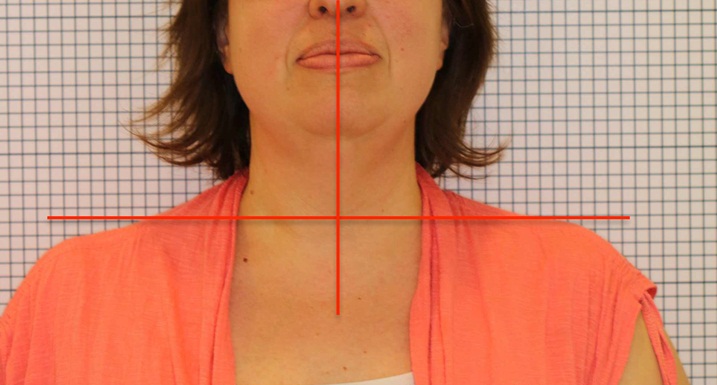
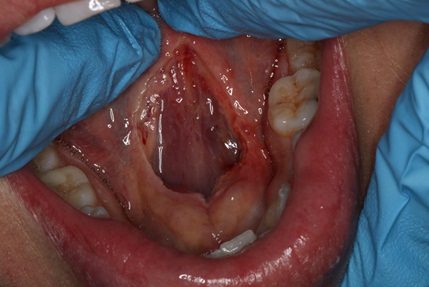
Post-Op Relief Topical Oil: I recommend using an oil rich in Vitamin K2 to assist in healing and reduce pain under the tongue. Walkabout Emu Oil is the best I’ve found and helps to reduce post-operative pain.
Measurements before and after surgery
Before tongue-tie surgery:
Opening with tongue suctioned to palate: 20mm
Tongue on roof of mouth: 35mm
Max jaw opening mouth: 50mm
Lower lip measure: 16mm
Upper lip measure: 20mm
After tongue-tie surgery:
Opening with tongue suctioned to palate: 29mm
Tongue on roof of mouth: 43mm
Max jaw opening mouth: 60mm
Lower lip measure: 14mm
Upper lip measure: 21mm
Lisp and speech pathology:
As an experienced speech pathologist, Michelle was able to do a self-assessment of her lisp. She produced a dentalised /s/ whereby her tongue pushed downwards on the lower front teeth and a slightly muffed /s/ sound was produced as the airflow was directed forward.
Usually, an /S/ sound should mean the tip of the tongue just comes off the top of the palate. Michelle was unable to correctly produce /s/ sound in this position prior to the tongue tie release. A tongue-tie may result in not being able to achieve correct tongue placement resulting in a ‘lisp’.
There are four types of lisp: Michele identified here own lisp. As an example here is two types of lips.
Interdental: ‘TH’ sound, where the tongue pokes through the teeth.
Lateralized lisp: where air flow comes out the side of the teeth.
Michelle’s own analysis describes the lack of control of the tongue’s side muscles. These are important hold the tongue in position whilst slightly releasing the tip of the tongue for correct airflow to make a /s/ sound. A tight lingual frenulum pulls the tongue and changes the shape of it for an /s/ production.
For more information on lisp you can read a full guide here
Four weeks after tongue-tie surgery – The remarkable recovery
Michelle’s life changed significantly after her tongue-tie surgery.
“My sleep length time improved straight away. I can now sleep 7 ½ hours to 8 hours on CPAP. There are still waking periods but can get straight back to sleep. Before I could never get to sleep.
I notice I can keep my mouth closed through the day. I use less paw-paw ointment on my lips because I’m not mouth breathing during the day. There is no longer need for afternoon naps, and I have plenty more energy and feel alert in the evenings. I can socialize through the week which I had not done for years.
My gut issues decreased, reflux has settled which I think was contributing to my night time waking.
I feel the front part of the tongue fits into my palate. At the back feels a bit crowded. My posture has improved; I can now get myself into straight posture before my neck begins to hurt. The back and neck pressure released almost immediately after the tie. My teeth clenching appears to have stopped (I need to confirm this) and my tooth sensitivity has ceased.
There have been no headaches or migraines, since the release. They have completely resolved.
I feel much calmer as a person. For instance, I burnt my hand, instead of panicking I put my tongue up and felt calm. I no longer feel anxious, and I have postponed my psychology sessions.
I’ve also lost 5 kg since the procedure. I don’t feel the cravings and dependence on sugar for energy.
My life has changed significantly since having the release. I would recommend anyone who thinks they may have a tongue-tie to investigate further.
I am continuing working with Sarah from Enhance Dentistry with an Orofacial Myofunctional Therapy program to achieve my goals. Most excitingly I can now produce /s/ and /z/ sounds with tongue in correct position.”
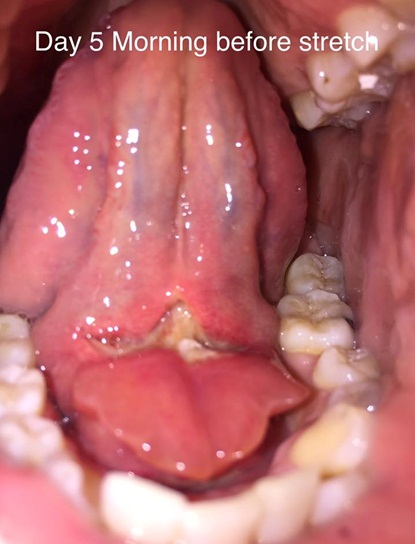
Tongue tie surgery recovery time
Generally, the wound can take between 2-7 days to heal. Post-op pain is common after the surgery. Michelle reported very little post-op pain. She took a course of codeine-panadol painkillers before treatment, 6hrs after and 6 hours after tongue tie surgery.
Some patients report significant soreness post op for weeks after surgery.
Post-Op Relief Topical Oil: I recommend using an oil rich in Vitamin K2 to assist in healing and reduce pain under the tongue.
Walkabout Emu Oil is the best I’ve found and helps to reduce post-operative pain
Tongue tie surgery types for adults
This treatment can be carried out without needing to have General Anesthetic and options are:
- Release of the frenum by laser with local anesthic or with topical anesthetic (gel) only
- Release of the frenum with scissors and local anesthetic.
- Release by electrocautery using a local anesthetic.
Tongue tie surgery complications
- Recurrence of lingual frenum can occur, especially in growing children. This may mean a revision is necessary in certain cases.
- Damage to surrounding structures of the floor of the mouth may end up in vessel or nerve damage. Always consult with your practitioner regarding potential risks and complications before surgery.
What is the cost of tongue tie surgery for adults?
Prices generally vary between $300-1200 for depending on the level of support and lead up treatment. A general anesthetic will increase the procedure cost significantly.
You can watch an adult tongue-tie release video with the team at Enhance Dentistry Brisbane below:
Do you have a question regarding adult tongue-tie release? Have you had the procedure performed? Leave your experiences in the comments below.
For more information on Dr. Lin’s clinical protocol that highlights the steps parents can take to prevent dental problems in their children: Click here.
Want to know more? Dr Steven Lin’s book, The Dental Diet, is available to order today. An exploration of ancestral medicine, the human microbiome and epigenetics it’s a complete guide to the mouth-body connection. Take the journey and the 40-day delicious food program for life-changing oral and whole health.
Click below to order your copy now:
US AMAZON
US Barnes & Noble
UK AMAZON
Australia BOOKTOPIA
Canada INDIGO








63 Responses
Thanks for the great information about oral surgery to release a tongue tie. I didn’t know that being tongue tied effects so many things like how the neuro-muscular system is intertwined with the brain and several other things. That makes sense and makes me wonder if I need the procedure because I feel a lot of pain from the bottom of my tongue. This all very interesting and I’ll soon find a local oral surgeon to check out my mouth.
Thank you for your feedback Sandra. Tongue-tie release definitely gives a lot of benefits when done correctly. It’s good to hear that you’ll have yours released soon!
Dear Dr. Lin,
I have tinnitus — and recently went to see Dr. Shirazi in LA and he said i was tongue tied and wanted to do surgery and I am scared.
http://tmjandsleeptherapycentre.com/dr-shirazi/.
Is he the right kind of person to do this surgery. He gave me no warning or pre op excercises… it kind of freaked me out.
Dr Lynn please help me find a qualified doctor to properly release my adult posterrior TT I’m 28 yet old It’s been a long time not being able to speak properly croocked teeth ect… Please please please can you refer me to anyone. Ear SW Pennsylvania please
Thanks a lot for the information. My tongue tie was released today, it hurts but I feel more better now. I was wondering about what to eat and what not to eat. There was a stitch after the surgery.
Hi Helen,
Main thing is to not irritate the wound. Stay away from acidic and spicy foods until it heals. But it should be quick!
Dr Steven Lin
Wow this is me!!
I start my journey in a couple of weeks at 48yrs.
Thank you for sharing
Thank you very kindly for your feedback. And congratulations on starting your journey!
Thankyou for sharing in such detail.
I had a frenotomy 3 years ago and didn’t do the stretches……..
Am going to be assessed for a 2nd frenotomy and have the pre and post op CST
I had the surgery on July 6th. My opening looked like the tongue picture on this site. I did all the exercises constantly (even tho it was so painful). Upon wakening each morning, my tongue felt like a ball. Had to stretch it immediately. The speech lady accused me of doing no exercises. Now it’s been 5 weeks and as it heals, it still has restrictions. Basically I went from severe to moderate. Toying with the idea of going back for her to do more laser. Love to hear how you made out..
Thank you Dr. Steven for sharing this useful article. I am 34 year old lady from india. I am also facing tongue tie problem which I have detected 4 year ago by searching at google. I do’t have any medical symptoms mentioned above but I have speech problem. I am unable to pronounce some word speak by tongue tip touching the teeth because my tongue has no sharp tip , it’s not oval as generally found. Due to this problem I sometimes feels very less confident to speak all of a sudden.some words slips. Is it possible to operate it at this age. Because sometimes I have to give lecture but due to this problem I feels low confidence. I am also feeling the problem of forgetting things. Is this related to this problem.
Hey there,
Yes, it’s absolutely safe. Tongue-tie release definitely gives a lot of benefits when done correctly. I suggest that you see a well trained professional first to further check on your condition before you undergo surgery. Good luck!
Hi Deepti,
I feel I have same issue regarding tongue tie and cannot pronounce R alphabet clearly if you don’t mind can you please let me know whom are you contacting on this and you can contact me on wajj567@gmail.com
I have read this article with interest and I have many of the physical problems listed eg poor sleep, low energy, anxiety, digestive issues and many TMJ and neck problems, plus anxiety and snoring. Is there someone in Adelaide who deals with this problem? I have heard that this problem is a genetic problem and can be passed down through the generations.
Riverside preventative dentistry
Thanks for sharing this informative health problem with some of us who are looking for solutions to our speech problem.
I will describ my symptoms like the ones mentioned above by Deepti from India. I also feel anxious sometimes and less confident to speak in public. I am aware of these issues and it makes me unconfortatle when giving lectures in front of my students. Sometimes, I feel like I am forgetting things.
Do you thing surgery can help in my case
Hi AJ,
Surgery can surely help. You will also want to see a well trained professional first before getting the procedure done. Good luck!
I’m 29 and a professional singer and voice over actor. I have constant headaches and fatigue. Yesterday, I registered with a new dentist and she diagnosed me as tongue tied! I was so surprised that I had never spotted this before. I’ve seen many ENT and Speech Paths in my life and couldn’t believe it was never identified. Interestingly, I can extend my tongue quite far and it does reach the top of my mouth, so even after being told I was tied, I was skeptical. But then the dentist pointed out: when I swallow, I push against my front teeth rather than the ‘spot’ above my teeth (where your tongue should go). Over the years, this has caused my teeth to push forward and flair out. How fascinating. I have surgery on the 5th and I’m so worried it might alter my voice or how I speak.
Ruth, Did you have the procedure done? Did they also cut the freulae attached to the bottom lip/gum at the base of the front teeth? My child’s oral surgeon is recommending that flap at the base of her mouth be cut to prevent recession around her bottom teeth. She’s a singer/actor so I’m wondering if that would affect her voice?
How did it go?? I am a soprano. And it looks like I need the same surgery. Freaking out a little…
Hi Kim,
Yes, it’s possible, speech pathologists can work right along side after the release in order to retrain tongue seal.
Chelsea
Community Manager
http://www.drstevenlin.com
Hi Ruth,
Voice alteration possible, speech pathologists can work right along side after the release in order to retrain tongue seal.
Chelsea
Community Manager
http://www.drstevenlin.com
This is a great article. I had my tongue tie released with laser in San Diego on Nov. 7 at age 40 and it’s healing well. I still have a bit of pain when I do the stretches, but my range of motion is so much more than before. I still can’t touch the tip of my tongue to the roof of my mouth when it’s wide open, but it’s SO much closer than before. I can now touch the outside of my back molars and my pain in my neck is significantly reduced. I have found myo-fascial massage of the floor of my mouth to be essential, along with my OMT appointments. I am actually putting together a mini-course on my Tongue Tie experience because I think more people need to know about the details and benefits of this relatively simple procedure!
Sarah ~ Where did you have your tongue-tie-release surgery? And by whom? I’m looking for a specialist who can help me. I don’t live in a very progressive area, so I will likely need to travel.
Were you in pain after the procedure? Were you able to talk and was your voice still the same? How do you feel overall.. I’m tongue tied and thinking of having the procedure done.. so love hearing about other people experiences after they had the procedure done.
Did you have this done yet? I am doing a documentry film on this subject and am looking for adults that are seeking treatment to film their journey. Please contact me if you are interested!
Iam having my release done April 16th in Chicago. My sister sent me this article and it explains so much of the issues I’ve had all of my life . Looking forward to starting the process of getting my energy back.
Interesting article. I had a lingual frenectomy done in April this year and am currently having the same pain again. Wondering if I should go in and have another one done?
This is unmitigated nonsense, Feeding Dr Lina’s ego and self importance. There is very little evidence for his claims The person in the photo has a completely normal lingual fraena.
By all means part with hard earned dollars for unnecessary intervention but see a medical specialist in the area of your concern and be sure they are motivated by your benefit not their hip pocket.
All hype no substance
I just got my tongue tie revised yesterday but I’m having some issues talking. It feels like I have something stuck under my tongue, even though I don’t. Is that a normal feeling or sensation? I also feel like right now I have lost some range of motion with my tongue.
How do you feel now? I’m thinking of getting my tongue tie released.. Are you talking now and is your voice still the same.. I’ve read quite alot of positive experiences after the procedure and people felt fine with minimal pain… Hope your doing better now.
I’m 21. I had my tongue-tie released 2 days ago by laser frenectomy. I have a couple of questions.
1. The surgeon said that stitches are not required – because the surgery was done by a laser, not a scalpel. Is it true?
2. It’s been 2 days since the surgery. I think that the cut is still open. It pains when I try to move my tongue. And online I read that tongue exercises are necessary to prevent the frenulum from reattaching. What should I do? When should I expect the pain to go away? Should I try to stretch my tongue even when I “think” the cut is open, and pains?
hello,
i read an article of your website, like i set the link here, i did cut accidentally tongue-tie, i had normal,,never problems but today i did cut accidentally. is any big issue in future in speak or sound of letters or anything like that?
thank you
best regards
beni
Hi.
It’s been 5 days since my tongu-tie surgery and my tongue is still very swollen. It’s like it’s double its normal size, I can’t really eat and I’m actually on liquid diet for all this time 🙁 How long does it take to heal?
I would go for a review with your practitioner, swelling can happen for varying amounts of time after surgery.
Hello everyone! I am making a documentry on this subject and looking for untreated adults that want to get a release and follow their journey. Please contact me @ jennybunnybee@gmail.com if anyone is interested. Also, I would love to connect with Dr. Lin if possible! I think we know some of the same people at the Breathe Inst. In Ca.
Hi Jennifer,
Your documentary sounds great. Can you contact us at info@drstevenlin.com
Dr. Steven Lin
Did you ever make this? I would love to watch it?
I would like to have myself, and my three children assessed. We all have these issues you are taking about. I have spent thousands on dead end help. This is the first time I have found a functional medicine dentist. Do you have a reputable list of referrals? That would follow the protocols on your website? I am in San Diego and would be willing to travel.
Myself and my two children got released two days ago. I would suggest to not do everyone at once like we did. It is a bit overwhelming.
Hi Joanne, thank you for sharing you’re right the recovery time can be a bit taxing. Best do it one by one so that the family can help the recovery process.
Namaste! Dr. I am from India.I am suffering from tongue tie I am 18 year old.I want to release my tongue tie.would you please tell me which option is better for releasing tongue tie laser or simple procedure?
Hi Manik,
In adults scissor release may be more appropriate, however, laser is also useful too.
Dr. Steven LIn.
Hello! Do you use Twitter? I’d like to follow you if that would be okay. I’m undoubtedly enjoying your blog and look forward to new posts. cbgdfebfdggbdkca
Hi Smith,
You may follow Dr. Lin on Twitter at this http://www.twitter.com/DrStevenLin. We’re glad that you are enjoying the articles.
Hope this helps, too.
Thanks!
Chelsea
Community Manager
http://www.drstevenlin.com
you’re truly a just right webmaster. The site loading speed is incredible. It kind of feels that you are doing any distinctive trick. In addition, The contents are masterpiece. you’ve performed a magnificent task in this subject! baacedkdefffceak
I am in arizona. should I go to an oral surgeon for this procedure? I am tongue tied for sure. I found out a couple years ago by my orthodontist.
Kolkata boasts of curvy women who are the most fantastic Kolkata Russian Escorts one would ever come across in their life. Thus, satisfying needs become easier as these women are gorgeous and have Goddesses like figure and skills. Try them for yourselves and you would know for yourself. The most beautiful women come in all shapes and sizes and this applies to the women of Kolkata too. They range from slim and tell to plumpy Indian curvy women. They are sexy and beautiful at the same time. They turn your wildest desires and fantasies into blooming realities which are hard to ignore. Come taste the beauty of Kolkata call girls and have a life-changing experience.
http://www.simranindependentescort.com/russian-escorts-in-kolkata.html
Hi, I’m wondering do you know, as I’m 17, can I have this done at a dentist/orthodontist on the nhs or would I still be required to pay a similar amount? My orthodontist did offer to do it a couple of years ago when I had my braces taken off but I was too scared at the time. Thanks.
I am not a professional, but it is important to find a therapist that is knowledgable and will work with you before and after the procedure.
I am a 35 year old woman who has a tongue tie and a narrow upper arch. I am scheduled for a frenectomy next week and I was wondering if I should also look into having my arch expanded to help me breathe more easily? I have sleep apnea and my tongue has scalloping from pushing against my teeth. I have an oral device and it has helped me get better quality sleep. I have trouble maintaining nasal breathing during the day, especially when exercising. How much would having my arch expanded help optimize breathing? Thanks so much!
My 19 year old daughter is about to have it done. She is extremely excited. I am wondering if it could possibly change the way she speaks in a negative way? She has no speech issue currently.
Hi Tania,
Yes, it is possible. But we highly encourage you to see a speech pathologists who can work right along side after the release in order to retrain tongue seal.
Thanks!
Chelsea
Community Manager
http://www.drstevenlin.com
This is some amazing information about tongue tied I can’t even stick my tongue out and it hurt to yell or to even talk it’s frustrating I can’t pronounce some words I’ve been waiting I’ve been looking for someone in Arkansas to do the surgery but I don’t know who to call and will I need dental insurance or regular Medicaid for the surgery
I have read Michelle’s story. My 15 year old daughter was born with mild tongue tie . It is now severe and she mirrors most of Michelle’s symptoms. The dental surgeon who we see last week thinks her tongue tie is not related to all of the other symptoms. I hope he is wrong and have I printed off Michelle’s story to show to the paediatrician tomorrow and she what she thinks. It will be a great relief if the tongue tie is the route of all problems as we will know then they are not separate issues and all symptoms will disappear once she has the surgery at the end of August. Thank you for sharing your story Michell.
The tongue tie can be a big problem at any age. The adults are more difficult to tolerate any kind of doctor’s interventions in this area.
How did a speech pathologist go so long without the surgery?
I am an adult who just had surgery for tongue tie. The doctor put stitches in, so even though the tongue tie is cut the tissue is still sewn together at the bottom towards the back of the tongue, not left open like in the photos above. I think this is restricting my tongue similarly to when I was tongue tied. Did the doctor screw this up? Will I need to have a revision?
Is it possible we can get some pictures of healing. In have seen many instances of a thick fibrotic scar afterwards and what seems greater restriction afterwards.
My 16 year old step-son was recently told by his dentist that he is tongue-tied. They want to do cautery to release it. The strange thing is that he has seen this dentist since he was a baby and it has never been mentioned till now. He also recently had his braces removed and was doing well, but at a recheck suddenly his bite is off. Is this related to tongue-tie? He is a mouth breather which I attributed to sinus issues. Should we get a second opinion with an ENT?
I would definitely get multiple opinions. I am no expert but an adult who underwent a frenectomy and regret it. If your son has no speech issues I would be cautious. Additionally, you should see an ENT if you can and perhaps see if you can exercise a more conservative approach (non surgical) and do some myofunctional therapy beforehand. It may help his symptoms. A lot of the research with tongue ties is in its infancy and I personally would be hesitant.
My 16 yo son’s dentist has blamed the frenum on his gum recession (3 spots) during ortho work. Sounds logical, but I’m curious, KC, what is your regret exactly (speech?), sloppy tongue…? Other than a tight neck, he has no other sx than the 3 teeth w recession. I’ve been searching for images showing when it’s nec and when it’s not… Is any attachment (frenum) okay?
This article def helped some…but 2nd opinion nec.
That was a great article on the surgery.