








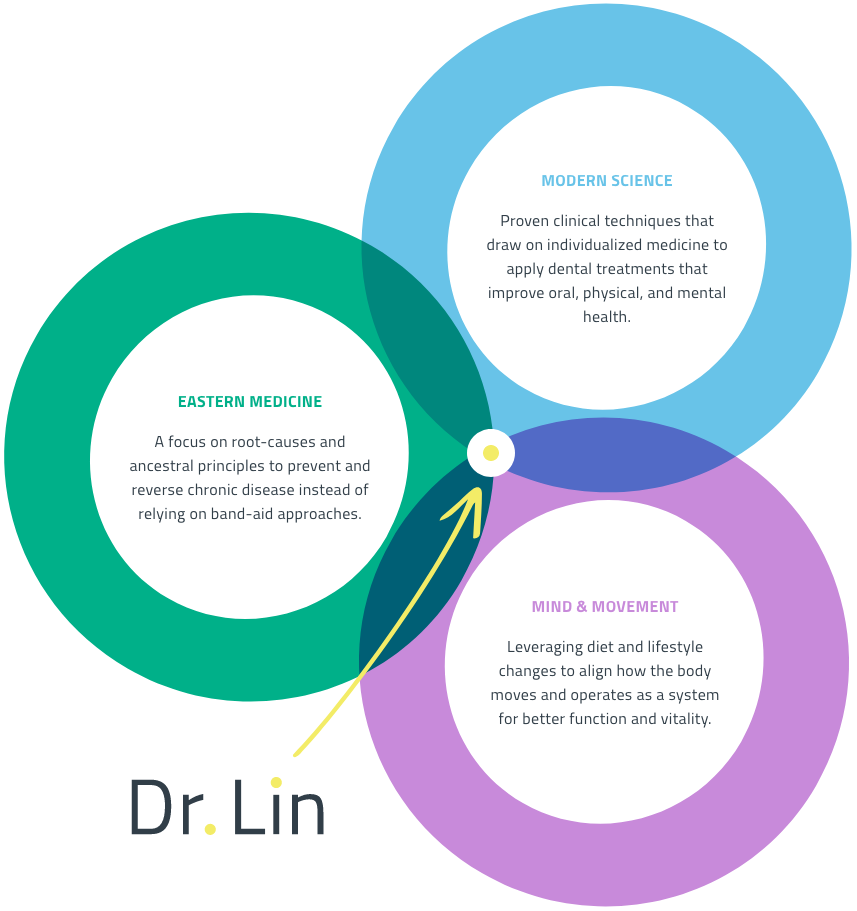
Your mouth reveals cardinal signs of your entire health. As a dentist I discovered that we’ve been making BIG mistakes in our approach to healthy teeth.
Food, NOT drills and needles, were the key to a better smile.

© 2023 Dr Steven Lin. All Rights Reserved.